Understanding CLL/SLL ICD-10 Codes: A Comprehensive Guide
What is CLL/SLL ICD 10?
Chronic lymphocytic leukemia (CLL) and small lymphocytic lymphoma (SLL) are both types of cancer that affect the lymphocytes, a type of white blood cell. In the ICD-10 coding system, CLL and SLL are classified under the same code, C91.1.
Code Information

ICD-10 code C91.1 is used to classify CLL and SLL, which are both types of lymphoid leukemia and lymphoma. This code is used for medical billing and coding purposes to accurately identify and document cases of CLL and SLL.
Diagnostic Related Groups (MS-DRG)
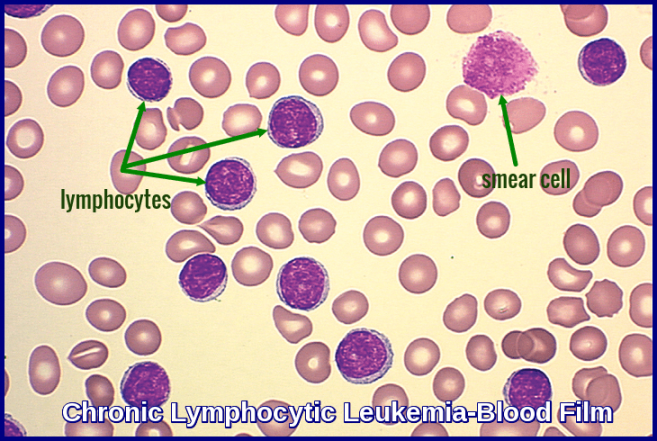
CLL and SLL fall under the category of malignant neoplasm of lymphatic and hematopoietic tissue in the MS-DRG system. This means that patients with CLL or SLL may be assigned to a specific DRG for billing and reimbursement purposes.
Convert to ICD-9 Code

In the ICD-9 coding system, CLL is classified under code 204.1, while SLL is classified under code 200.5. It is important to accurately convert these codes to the corresponding ICD-10 code to ensure proper documentation and billing.
Code History
The ICD-10 code C91.1 for CLL and SLL was introduced in October 2015 as part of the transition from ICD-9 to ICD-10 coding systems. This transition was aimed at improving the accuracy and specificity of medical coding and classification.
Approximate Synonyms
Some approximate synonyms for CLL and SLL include chronic lymphocytic leukemia, small lymphocytic lymphoma, and lymphocytic leukemia of the small lymphocytic type. These terms are used interchangeably to describe these types of cancer.
Clinical Information
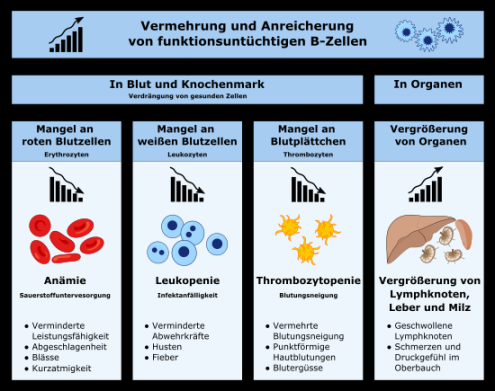
Patients with CLL/SLL may present with symptoms such as enlarged lymph nodes, fatigue, weight loss, and frequent infections. Diagnosis is typically confirmed through blood tests, imaging studies, and bone marrow biopsy.
Causes
The exact cause of CLL/SLL is unknown, but genetic factors, environmental exposures, and immune system abnormalities may play a role in the development of these cancers. Risk factors include age, family history, and certain genetic mutations.
Symptoms
Symptoms of CLL/SLL may include fatigue, enlarged lymph nodes, night sweats, weight loss, and frequent infections. Some patients may be asymptomatic and diagnosed incidentally through routine blood tests.
Diagnosis
Diagnosis of CLL/SLL is based on a combination of clinical presentation, blood tests (such as complete blood count and flow cytometry), imaging studies (such as CT scans and PET scans), and bone marrow biopsy. A confirmed diagnosis is essential for appropriate treatment planning.
Treatment
Treatment for CLL/SLL may include watchful waiting, chemotherapy, immunotherapy, targeted therapy, radiation therapy, and stem cell transplantation. The choice of treatment depends on the stage of the disease, the patient’s overall health, and other individual factors.
Conclusion
CLL/SLL is a type of cancer that affects the lymphocytes and is classified under the ICD-10 code C91.1. Accurate diagnosis and classification of CLL/SLL are essential for appropriate treatment and management. Patients with CLL/SLL may present with a variety of symptoms and may require a multidisciplinary approach to care.
FAQs
1. What is the difference between CLL and SLL?
In CLL, the cancer cells are primarily found in the blood and bone marrow, while in SLL, the cancer cells are mainly found in the lymph nodes.
2. Is CLL/SLL curable?
While CLL/SLL is generally considered incurable, many patients can live for years with the disease with appropriate treatment and management.
3. Are there any risk factors for developing CLL/SLL?
Age, family history, and certain genetic mutations are known risk factors for CLL/SLL.
4. What is the prognosis for patients with CLL/SLL?
The prognosis for CLL/SLL varies depending on the stage of the disease, the patient’s overall health, and other individual factors.